If you’re dealing with chronic joint pain or a stubborn injury and want to avoid surgery, you’ve probably come across stem cell injections as a possible solution. The claims can sound remarkable, but sorting fact from marketing is genuinely difficult. Evidence from systematic reviews suggests these treatments may offer modest improvements in pain and function compared to placebo, though the certainty of that evidence remains low and joint regeneration is not reliably demonstrated. This article gives you a grounded, evidence-based picture of what stem cell injections can realistically offer, what the risks look like, and how to think clearly about whether they might fit your situation.
Table of Contents
- What are stem cell injections and how are they used?
- How do stem cell injections work for joint pain and injury?
- What can you really expect? Evidence for pain relief, function, and risks
- Why outcomes and safety can really vary: Clinic, product, and patient factors
- The real story: What most people miss about stem cell injections for joint pain
- Explore non-surgical options with Nortex Tissue Regeneration
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Set realistic expectations | Stem cell injections usually help symptoms but don’t guarantee joint regeneration. |
| Clinic approach matters | Outcomes depend heavily on product type, clinic protocol, and patient-specific factors. |
| Safety demands diligence | Serious risks are uncommon but you should still vet your provider closely. |
| Ask the right questions | Knowing details about the procedure and evidence can help you make informed choices. |
What are stem cell injections and how are they used?
With an understanding of their appeal and marketing, let’s dig deeper into how stem cell injections actually might work inside your body.
Stem cell injections involve harvesting living cells from your own body or a donor source, processing them, and then injecting them into a damaged joint, tendon, or surrounding tissue. The goal is to use those cells’ natural signaling capacity to calm inflammation, support tissue repair, and improve how the joint functions. This is a genuinely different approach from cortisone shots, which suppress inflammation chemically but do nothing to promote healing.

The most commonly used cell type in orthopedic settings is the mesenchymal stem cell (MSC). These cells can be sourced from several places in the body, including bone marrow drawn from the hip, fat (adipose) tissue from the abdomen, or birth-related tissues like amniotic fluid or placental membranes. Each source produces a somewhat different cellular environment with varying concentrations and biological properties. Understanding how stem cells heal joints at a biological level helps clarify why source and preparation matter so much.
Here’s what the procedure typically looks like:
- Cell harvesting: Bone marrow aspiration or fat tissue removal is performed under local anesthesia, usually as an outpatient procedure.
- Processing: The harvested material is spun in a centrifuge to concentrate stem cells and other regenerative components.
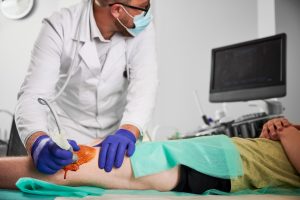
- Image-guided injection: Using ultrasound or fluoroscopy, the provider injects the processed cells directly into the affected area for accuracy.
- Recovery: Most patients return to light activity within a few days, though full response to treatment takes weeks to months.
What makes this area complicated is that product heterogeneity across clinics is significant. Cell counts, purity levels, processing methods, and even what qualifies as a “stem cell” product can vary enormously from one facility to the next. A product labeled “stem cell therapy” at one clinic may look entirely different from what another offers. For a thorough overview of what to expect procedurally, our stem cell treatment guide walks through each step in detail. You can also find safe non-invasive options if you’re still in the early stages of evaluating your choices.
Pro Tip: Always ask your provider about the exact cell source, preparation method, and supporting evidence behind their specific product. “Stem cell injection” is not a standardized treatment, and the details matter a great deal for your outcome.
How do stem cell injections work for joint pain and injury?
Now that you know how these injections are supposed to work, let’s look at evidence on whether they actually deliver the promised benefits.
The biological theory behind stem cell injections is compelling. When MSCs are introduced into a damaged joint, they are thought to release signaling molecules called cytokines and growth factors that reduce inflammation and may encourage local tissue cells to repair. Think of it less as the stem cells directly building new cartilage and more as them sending chemical instructions to surrounding tissue to behave in a more regenerative way.
Lab studies have consistently shown these signaling effects in controlled settings. The challenge is that the human joint environment is far more complex than a petri dish. Factors like joint loading, immune responses, existing tissue damage, and the patient’s overall biology all influence whether those same repair signals translate into meaningful clinical improvement.
“Effectiveness varies; hurdles remain unresolved, including risks like immune rejection and product variability.” This is a consistent finding across orthopedic reviews, reminding us that promising lab data does not automatically mean reliable patient outcomes.
Orthopedic stem cell reviews consistently highlight that while the proposed mechanisms are scientifically sound in principle, real-world results are variable and not yet fully predictable. There are also legitimate safety concerns worth knowing, including localized immune responses at the injection site and, in rare cases, theoretical risks of abnormal tissue growth when cells behave unexpectedly.
Here’s a summary of proposed mechanisms versus the current strength of supporting evidence:
| Proposed mechanism | Lab evidence | Human clinical evidence |
|---|---|---|
| Reduction of joint inflammation | Strong | Moderate, inconsistent |
| Cartilage repair or regeneration | Moderate in animal models | Weak to absent in RCTs |
| Tendon and ligament healing | Moderate | Limited, early-stage |
| Pain signal modulation | Moderate | Modest improvement vs. placebo |
| Reduction of inflammatory cytokines | Strong | Moderate, varies by product |
For more detail on stem cell therapy details and what treatment at a specialized clinic involves, we outline our protocols and the evidence we rely on. The gap between lab findings and reliable stem cell joint healing outcomes in humans is one of the most important things to understand before you commit.
What can you really expect? Evidence for pain relief, function, and risks
Since not all clinics or products are the same, let’s break down the key variables that can heavily influence your outcome.
Here is the honest picture: most people who receive stem cell injections for joint pain experience modest improvements in pain and sometimes function compared to placebo. Best available evidence from systematic reviews shows this pattern clearly for knee osteoarthritis, the most studied joint condition. Structural improvements, meaning actual cartilage regrowth visible on MRI, are not reliably demonstrated.
A 2026 systematic review and meta-analysis of randomized controlled trials reinforced this: pain scores improved and some functional gains were observed, but MRI-based structural benefits were non-significant. Serious complications were uncommon across the studies reviewed, though researchers noted that long-term safety data is still limited.
Statistic to keep in mind: Serious adverse events across clinical trials are infrequent, but true long-term safety for stem cell injections in joints remains uncertain because most trials follow patients for less than two years.
How do stem cell injections stack up against other common options? Here’s a practical comparison:
| Treatment | Primary benefit | Structural repair | Evidence strength | Common risks |
|---|---|---|---|---|
| Stem cell injection | Pain relief, some function | Not reliably shown | Low to moderate | Injection site pain, immune response |
| PRP injection | Pain relief, anti-inflammatory | Limited | Moderate | Injection site flare |
| Cortisone injection | Fast pain relief | None, may worsen over time | High for short-term | Tissue weakening with repeated use |
| Surgery (e.g., knee replacement) | Structural correction | Yes | High | Surgical risks, long recovery |
For a closer look at how PRP for knees compares in terms of evidence and experience, that resource gives specific context for North Texas active adults. Understanding the limits of both approaches will help you have a much more productive conversation with your provider.
Before proceeding with stem cell injections, consider asking your specialist these key questions:
- What is the exact source of the cells used in my treatment?
- How are the cells processed, and what is the typical cell count in each injection?
- What peer-reviewed evidence supports this specific product for my condition?
- What outcomes do your patients typically experience, and how do you track them?
- What are the realistic timelines for noticing improvement?
- What are the alternative non-surgical treatments if this approach doesn’t produce results?
These questions aren’t meant to challenge your provider; they’re meant to help you make a genuinely informed decision about your own body.
Why outcomes and safety can really vary: Clinic, product, and patient factors
Understanding these nuances makes all the difference in decision-making, but what should you take away as the bottom line?
One of the most frustrating realities of stem cell injections is that two people with similar joint conditions can have very different outcomes, and that variation often comes down to factors that have nothing to do with how hard they tried or how carefully they followed aftercare instructions. Product heterogeneity and protocol differences are major sources of variability across clinical results. This means the evidence from one clinic’s approach may not apply to what another clinic offers, even if both call it “stem cell therapy.”
Here are the key variables that influence your outcome:
Clinic and provider variables:
- Cell source: bone marrow versus adipose versus birth tissue products have different biological profiles
- Processing method: the centrifuge speed, time, and additives used change the final product significantly
- Injection technique: image guidance improves accuracy and is associated with better outcomes
- Provider experience: the number of procedures performed and protocol adherence matter
Product variables:
- Cell count and concentration in the final injectable
- Whether the product contains true stem cells or a broader mix of regenerative cells
- Regulatory status of the product used (FDA oversight varies significantly)
Patient variables:
- Age and baseline health affect how well cells survive and signal after injection
- Severity of joint damage: early to moderate arthritis generally responds better than end-stage joint destruction
- Immune health, prior injections, and medications can all influence results
Comparing PRP vs. stem cell therapy is a useful exercise because it helps you understand where each therapy’s strengths lie based on your specific diagnosis. Our bone marrow cell therapy details page explains the specific approach we use and why we favor it for certain conditions. You may also find it helpful to review pain management alternatives if you want a broader context before settling on a treatment path.
Serious adverse events are infrequent based on current trial data, but researchers are clear that long-term and rare risks remain unknown. This is not a reason to avoid the therapy outright. It is a reason to choose a clinic that tracks outcomes systematically and maintains transparency about what they know and what they don’t.
Pro Tip: Reliable clinics will document their protocols, participate in outcomes registries, and be honest about where the evidence is strong and where it is still emerging. If a provider promises guaranteed regeneration or avoids your detailed questions, that is a significant warning sign.
The real story: What most people miss about stem cell injections for joint pain
Here is the candid perspective we share with patients who come to us after spending months researching options online: the gap between what stem cell injections are marketed to do and what current evidence reliably shows is meaningful, but that doesn’t mean the therapy lacks value. It means the conversation needs to be different.
Most people arrive hoping for regeneration. They picture cartilage growing back, a joint restored to its twenties-era condition. That hope is understandable, especially when you’re an active adult in North Texas who wants to keep running, hiking, or playing your sport. But the honest clinical picture is that the primary benefit, when there is one, is symptom improvement, particularly pain reduction and better daily function. That is genuinely valuable. It’s just not the same thing as structural repair.
The most commonly missed insight is that “stem cell therapy” is not one thing. We’ve seen patients who received a procedure at one clinic and were told it didn’t work, come to us and respond well to a different protocol. The cell source, preparation, and injection technique created entirely different biological conditions. Assuming your past experience with a generic product defines what the therapy category can do is a significant error.
“Benchmark your expectations around symptom improvement, not miracle cures.” This mindset shift changes everything about how patients evaluate their results and decide on next steps.
Hard-won clinical wisdom tells us that the best outcomes come from combining evidence-based protocols with honest patient selection. Not everyone is a good candidate. Someone with severe bone-on-bone arthritis and significant structural loss will likely need a different conversation than someone with early osteoarthritis and persistent pain that hasn’t responded to physical therapy or anti-inflammatory treatment. Deciding between options is exactly the kind of decision covered in our detailed PRP vs. stem cell therapy decisions guide.
Pro Tip: Demand specifics. Ask your provider for published trial results that match the exact product type and injection method they plan to use for your condition. Generic references to “stem cells working” are not sufficient justification for a procedure that costs thousands of dollars and introduces biological material into your joint.
Explore non-surgical options with Nortex Tissue Regeneration
At Nortex Tissue Regeneration, we work with active adults across North Texas who want real answers, not just optimistic marketing. Our approach to stem cell therapy is grounded in evidence-based protocols, and we also offer PRP therapy as a well-supported alternative or complementary option depending on your specific diagnosis and goals. We believe you deserve a personalized evaluation that looks honestly at your imaging, your history, and your activity goals before recommending any treatment.
If you’re ready to explore your regenerative healing options with a team that prioritizes transparency and outcomes over promises, we invite you to schedule a consultation. We’ll walk you through exactly what the evidence supports for your condition and help you make the decision that fits your life.
Frequently asked questions
Are stem cell injections a permanent fix for joint pain?
No. Most studies show modest short-term relief in pain and function, but evidence emphasizes symptom improvement rather than lasting joint regeneration. Repeat treatments may be needed as effects diminish over time.
Do all clinics use the same type of stem cells?
No. Cell types and preparation methods vary widely between facilities and significantly affect both outcomes and risk profiles. Major heterogeneity in product type means that one clinic’s “stem cell injection” can be biologically quite different from another’s.
What are the main risks of stem cell injections?
Injection-site pain or swelling are the most commonly reported side effects. Serious complications remain infrequent across clinical trials, but infection, immune response, and theoretical long-term risks are possible and should be part of your informed consent discussion.
How do stem cell injections compare to PRP or cortisone shots?
Some trials show modest pain improvement with stem cells, similar to or slightly better than placebo, but structural benefits are not reliably demonstrated on imaging. Cortisone works faster for pain but does not support healing. PRP has a moderate evidence base for certain conditions and carries a well-understood safety profile.
Should active adults consider stem cell injections over surgery?
They may serve as a reasonable non-surgical alternative when conservative treatments have not provided enough relief, particularly in early to moderate joint disease. Results are variable, and the best outcomes come from working with an experienced provider who evaluates your specific condition thoroughly before recommending any treatment path.