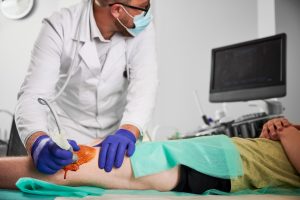
If you train hard, compete regularly, or simply refuse to let joint pain dictate what you can do, you have probably wondered whether cell therapy is the real deal or just a well-marketed shortcut. The science is more nuanced than most clinics advertise, and understanding it clearly gives you a significant advantage. Cell therapy does not simply mask pain. It may actively shift the inflammatory environment inside an injured joint, influence tissue repair signals, and support structures like cartilage and tendons in ways that conventional treatments cannot. This guide covers what current evidence actually shows, who responds best, what the risks are, and how to ask the right questions before committing to any treatment.
Table of Contents
- How cell therapy works in joint recovery
- What the evidence shows for pain, function, and joint health
- Nuance and key variables: Who might benefit most from cell therapy?
- Safety, risks, and what to ask your provider
- The perspective: Why realistic expectations and the right questions make all the difference
- Finding the right cell therapy provider in North Texas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Focus is on environment | Cell therapy works by changing inflammation and aiding repair rather than just masking pain. |
| Evidence is evolving | Currently, cell therapy shows modest improvements in pain and function, with benefits varying by joint and injury profile. |
| Safety requires questions | Serious side effects are rare, but understanding risks and product quality is essential for safe recovery. |
| Personalization matters | Patients with strong inflammation may see more benefit, so treatment should be individualized. |
How cell therapy works in joint recovery
The first thing to understand is that cell therapy is not a single treatment. It is a category of biologic interventions that uses living cells, most often mesenchymal stem cells (MSCs) derived from bone marrow, adipose tissue, or umbilical cord tissue, to influence how your body responds to injury or degeneration.
When cells are introduced into a damaged joint, most of them do not permanently “take root” and grow new tissue. That is a common misconception. What they primarily do is act as biological communicators. They release proteins, growth factors, and signaling molecules that change the local environment of the joint. This process is called paracrine signaling, and it is responsible for most of the therapeutic effects observed in research settings.
Here is what cell therapy can do inside an injured joint:
- Modulate inflammation. Chronic joint inflammation drives cartilage breakdown and pain. Injected MSCs release anti-inflammatory cytokines that can interrupt this cycle and create a more favorable healing environment.
- Stimulate matrix remodeling. The extracellular matrix, the structural scaffolding of cartilage and tendons, is influenced by growth factors secreted by therapeutic cells. This may slow degeneration and support repair.
- Regulate immune responses. MSCs can dampen overactive immune activity within the joint, which is particularly relevant for conditions like osteoarthritis (OA), where the immune system contributes to tissue damage.
- Support resident cell activity. Rather than replacing damaged cells outright, injected cells may activate the joint’s own repair cells, prompting them to work more efficiently.
Research into MSC biology confirms that cell therapy changes the joint environment through inflammation control, matrix remodeling, and immune signaling, and that outcomes extend beyond simple symptom control. Understanding how stem cells repair joints at this mechanistic level also explains why results take weeks to months to fully develop. You are not numbing the joint. You are asking the body to rebuild and recalibrate.
“The therapeutic potential of MSCs in joint conditions lies less in direct tissue replacement and more in their capacity to orchestrate a more favorable local biological environment through secreted factors and immune modulation.”
This distinction matters enormously when setting realistic expectations. Cell therapy is not a magic cure. But it is also not just a pain reliever in disguise.
What the evidence shows for pain, function, and joint health
Now that you understand the biological rationale, it is fair to ask: what do the clinical studies actually show? The honest answer is that results are encouraging but not conclusive at the highest levels of evidence.
| Outcome | What evidence shows | Evidence quality |
|---|---|---|
| Pain reduction | Moderate improvement over placebo in several trials | Low to moderate certainty |
| Physical function | Improvements in mobility and activity scores | Low to moderate certainty |
| Quality of life | Positive trends reported across multiple studies | Low certainty |
| Cartilage regrowth | Limited or inconsistent structural changes on MRI | Very low certainty |
| Long-term durability | Some cohorts show gains up to 4 years | Limited control data |
For knee osteoarthritis specifically, stem cell injections may improve pain and function over placebo, though the evidence is currently rated as low certainty due to small study sizes and variability in protocols. That does not mean it does not work. It means we need more well-designed trials to confirm how consistently it works and for whom.

For athletes dealing with soft tissue injuries, the data is more promising in some respects. A four-year observational cohort reported lasting improvements in pain and function for patients treated with MSCs for partial rotator cuff tears. No control group was used, which limits conclusions, but the durability of gains across four years is clinically meaningful.
Here is how to interpret outcomes data when evaluating any cell therapy study:
- Look at both pain scores and functional outcomes. A treatment that reduces pain by 20% but does not restore your range of motion may not be enough for an active athlete. Functional improvement is the more relevant metric for most people reading this.
- Check for a control group. Studies without placebo controls cannot rule out the possibility that improvement was due to the injection procedure itself, natural recovery, or expectation effects.
- Consider the follow-up period. Many studies report results at 3 to 6 months. If your goal is long-term joint health, ask what the data shows at 12, 24, or 48 months.
- Understand what “statistically significant” means. A statistically significant result means the change was unlikely to be random. It does not automatically mean the change was large enough to noticeably affect your daily life.
Learning about the stem cell therapy process in detail, and comparing it to other biologic options by reviewing PRP vs stem cells in studies, helps you see how these treatments stack up against each other and against more conventional approaches.
Pro Tip: When evaluating your own response to cell therapy, do not rely solely on pain ratings. Track your functional milestones, such as how far you can walk, how high you can raise your arm, or how well you can handle your sport-specific movements. These measures tell a fuller story.
Nuance and key variables: Who might benefit most from cell therapy?
This is the question that matters most for your decision. The evidence does not support the idea that cell therapy works equally well for every patient or every joint condition. Several variables meaningfully influence how likely you are to benefit.
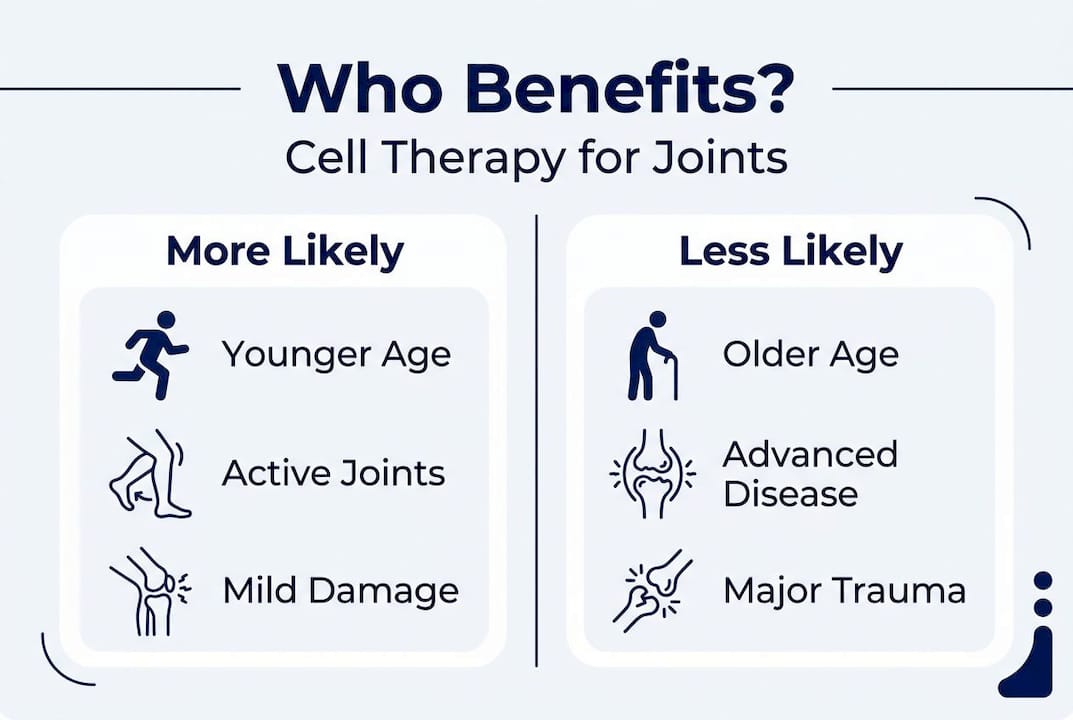
| Variable | More likely to benefit | Less likely to benefit |
|---|---|---|
| Age | Younger adults with active biology | Older adults with advanced joint breakdown |
| Injury type | Acute soft tissue, partial tears, early OA | Bone-on-bone arthritis, complete tendon rupture |
| Severity | Mild to moderate degeneration | End-stage joint disease |
| Inflammatory status | Active synovitis present | Purely mechanical joint damage |
| Overall health | Good metabolic health, non-smoker | Uncontrolled diabetes, systemic inflammation |
Consider two real-world scenarios. A 32-year-old recreational soccer player with a partial ACL tear and mild knee swelling is dealing with an acute inflammatory injury in a joint that still has significant healing capacity. Cell therapy in this context has a supportive biological environment to work with. Compare that to a 67-year-old with bilateral knee osteoarthritis rated as severe on X-ray, where cartilage is largely absent and the structural damage is extensive. The biology is very different, and so are the expected outcomes.
One of the more compelling recent findings involves patients with knee OA and an active inflammatory condition called synovitis, which is inflammation of the joint lining. A double-blind RCT studying UC-MSCs found significant clinical improvements and MRI changes in the synovium at six months for this specific patient group. This is an important insight: the presence of detectable inflammation may actually make you a better candidate for cell therapy, not a worse one.
Key factors to discuss with your provider when evaluating cell therapy variables include:
- The source of the cells being used (bone marrow, adipose, or umbilical cord derived)
- The preparation method and concentration of cells in the final product
- Whether imaging confirms active inflammation in the target joint
- Your injury timeline and previous treatments attempted
Pro Tip: If your imaging or physical exam suggests active synovitis, bring that finding specifically to your provider when discussing cell therapy. The latest research suggests this inflammatory phenotype may respond particularly well to MSC injections.
Safety, risks, and what to ask your provider
Cell therapy is generally considered a low-risk procedure, but “low risk” is not the same as “no risk.” You deserve a clear picture of what is known, what is uncertain, and what to ask before agreeing to any treatment.
Known risks include:
- Temporary soreness or swelling at the injection site, typically resolving within days
- A small risk of infection with any intra-articular (into the joint) injection
- Rare risk of septic arthritis, a serious joint infection requiring immediate treatment
- Procedure discomfort, particularly with bone marrow aspiration if that is the cell source
Areas of ongoing uncertainty:
The Cochrane review on cell therapy safety notes that serious adverse events were infrequent across studies but that rare or theoretical risks remain poorly characterized due to limited reporting. This is honest, not alarming. It means the field is still maturing and post-treatment surveillance is genuinely important.
A second major constraint involves standardization. Differences in cell sources, preparation methods, and dosing across clinics and studies make it difficult to compare outcomes or guarantee consistency. Not all cell therapies are created equal, and the quality of the product matters enormously.
“Patients considering cell therapy deserve transparent communication about what is known, what remains uncertain, and what safeguards are in place at the facility providing their care.”
Before proceeding, ask your provider the following questions:
- What is the source of the cells used in this treatment, and how are they prepared?
- What adverse events have been reported in your clinic, and how do you manage complications?
- How do you determine the appropriate dose and concentration for my specific injury?
- What follow-up protocol do you use after treatment, and how do you track outcomes?
- How does this approach compare to other options, including cell therapy safety versus other options like PRP or prolotherapy, for my injury type?
These are not skeptical questions. They are smart ones. A qualified provider will welcome them.
The perspective: Why realistic expectations and the right questions make all the difference
We want to be candid with you about something the marketing around regenerative medicine often glosses over. There is a real gap between the optimism that clinical experience sometimes generates and the current certainty that the research literature supports. Contrasting perspectives on cell therapy reveal a consistent pattern: clinicians and patient advocates often report meaningful results while systematic evidence reviews emphasize low certainty and limited standardization. Both can be true simultaneously.
From our experience working with active adults and athletes in North Texas, the patients who fare best with cell therapy are not necessarily those with the most severe injuries. They are the ones who come in with clear goals, realistic timelines, and a commitment to the full recovery process, including physical therapy, load management, and lifestyle adjustments that support tissue healing.
Cell therapy is most powerful as part of a strategy, not as a standalone fix. Pairing it with targeted rehabilitation, appropriate activity modification, and regular provider follow-up produces better outcomes than relying on a single injection to do all the work. We have seen patients experience genuine and lasting improvements in joint function. We have also seen patients who expected immediate, complete relief and felt disappointed when recovery took months. Setting those expectations honestly, before treatment, is part of delivering real care.
Understanding what drives better cell therapy results at a process level empowers you to be an active participant in your recovery rather than a passive recipient. Ask about the evidence. Ask about your specific phenotype. Ask what success looks like in measurable terms. These conversations lead to better outcomes, and they distinguish quality providers from those offering generic protocols to everyone who walks through the door.
Finding the right cell therapy provider in North Texas
At Nortex Tissue Regeneration, we approach every consultation from an evidence-based, patient-first perspective. We know that active adults and athletes in North Texas deserve more than a one-size-fits-all injection protocol. Our team evaluates your injury profile, imaging findings, inflammatory status, and recovery goals before recommending any treatment pathway.
If you are considering biologic treatments, exploring your options for North Texas stem cell therapy with a specialized provider is the most important first step. We also offer PRP therapy options for patients whose injury type and response profile make platelet-rich plasma a stronger fit. Every recommendation we make is tied to your specific clinical picture, not a treatment menu. If you are ready to have a candid, informed conversation about what cell therapy can realistically offer for your joints, we are here to help you navigate that decision with clarity and confidence.
Frequently asked questions
Does cell therapy regenerate cartilage in arthritic joints?
Current research suggests most benefits relate to reducing inflammation and supporting tissue repair rather than true cartilage regrowth. MSC biology evidence confirms that cell therapy alters the joint environment but does not consistently produce new cartilage tissue.
How long do improvements from cell therapy last?
Some studies report sustained pain and function gains for several years, but long-term durability varies with injury type and individual response. Four-year cohort findings for rotator cuff injuries showed maintained benefits, though the absence of a control group limits how firmly we can interpret those results.
Are cell therapies safe?
Studies show a low incidence of serious adverse events, but rare risks and differences in cell preparations remain important unknowns. Cochrane data shows that serious adverse events were infrequent, though uncertainties about rare or theoretical risks persist due to limited long-term reporting.
Which joint injuries benefit most from cell therapy?
Joint injuries with a strong inflammatory component, particularly those with active synovitis, may see the most benefit according to recent clinical trials. RCT data for UC-MSCs found the most significant improvements in osteoarthritis patients where synovial inflammation was confirmed on imaging.
Recommended
- Step-by-step stem cell treatment guide for joint recovery
- How stem cells heal joints: Evidence and real answers
- Stem Cell Therapy – Nortex Tissue Regeneration
- PRP vs Stem Cell Therapy: Which One Makes Sense for You? – Nortex Tissue Regeneration
- How to Speed Up Recovery After Physical Therapy or Surgery – Lunix