Many active adults and athletes in North Texas assume that once joint pain becomes severe enough to limit movement, surgery is the only real path forward. That assumption is increasingly challenged by a growing body of clinical evidence. Regenerative treatments, including platelet-rich plasma (PRP) and stem cell therapies, work with your body’s own biology to reduce inflammation, support tissue repair, and restore functional mobility without an operating room. This article walks you through how these therapies work, what the research actually shows, who benefits most, and how to combine treatment with smart rehab for lasting results.
Table of Contents
- What are regenerative treatments and how do they work?
- Evidence: How regenerative therapies improve mobility
- Why methodology and patient selection influence results
- Integrating regenerative treatments with rehab and load management
- What most guides miss about regenerative mobility treatments
- Explore advanced regenerative therapy options in North Texas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Science-backed mobility gains | Regenerative treatments can improve joint mobility by enhancing your body’s repair environment, reducing pain, and supporting function. |
| Best for early joint changes | Results are most pronounced when applied early in the degenerative or injury process, especially for mild-to-moderate conditions. |
| Methodology matters | Treatment outcomes depend on specific protocols, patient matching, and integration with rehabilitation and load management. |
| Manage expectations | These therapies reliably improve function and pain but do not guarantee cartilage regrowth or complete reversal of severe damage. |
| Holistic care approach | Combining regenerative interventions with rehab and healthy activity maximizes mobility and long-term joint health. |
What are regenerative treatments and how do they work?
With the common belief about surgery dispelled, let’s look at what regenerative treatments actually do inside your joints.
Regenerative treatments, often called orthobiologics, are therapies derived from your own body or from biologic sources. The most widely used options include PRP, bone marrow concentrate, and adipose-derived stem cells. Each one works differently at the cellular level, but they share a common goal: shifting the joint environment away from chronic breakdown and toward repair.
Healthy joints rely on a delicate balance between tissue breakdown and repair. In conditions like osteoarthritis or tendon injury, that balance tips toward degeneration. Chronic inflammation floods the joint space, cartilage thins, and the surrounding structures, including the synovium and tendons, begin to deteriorate. Regenerative therapies intervene in that cycle.
Regenerative orthobiologic approaches aim to improve mobility by modulating the joint’s underlying biology, targeting endogenous repair mechanisms and reducing chronic, whole-joint pathology such as inflammation and degeneration that drive pain and stiffness. Put simply, these therapies don’t just mask symptoms. They try to change the conditions that cause them.
The key mechanisms researchers are studying include:
- Growth factor signaling: PRP releases concentrated growth factors that stimulate cell proliferation and tissue repair at the injection site.
- Immunomodulation: Certain stem cell preparations help regulate the immune response inside the joint, reducing the inflammatory signals that drive cartilage breakdown.
- Cellular reintegration: Bone marrow and adipose-derived cells may support the local repair environment by interacting with resident joint cells.
- Synovial environment shifts: Regenerative therapies may improve functional mobility by shifting joint environments, including synovium, cartilage, and tendon interfaces, toward repair through growth-factor signaling and immunomodulation.
Expert insight: Regenerative treatments work best when they are integrated with load management and rehabilitation, not used as a standalone fix. The biology of joint repair is supported, not replaced, by the therapy.
Pro Tip: Not all joint pain comes from cartilage damage. Synovitis, tendon involvement, and subchondral bone changes all contribute to stiffness and reduced mobility. A thorough evaluation should assess the whole joint, not just cartilage thickness. You can read more about how stem cells heal joints and explore a detailed stem cell treatment guide if you want to understand what the process looks like from start to finish.
Evidence: How regenerative therapies improve mobility
Now that we understand the basics, let’s see what the research shows about real mobility gains.
The most studied regenerative treatment for joint mobility is PRP, particularly for knee osteoarthritis. Multiple meta-analyses and randomized controlled trials have measured outcomes using validated tools like the WOMAC (Western Ontario and McMaster Universities Osteoarthritis Index) and the VAS (Visual Analog Scale for pain). These aren’t subjective impressions. They are standardized measures of pain, stiffness, and physical function that translate directly to how well you move through your day.
PRP has evidence of improving patient-reported pain and function in degenerative conditions like knee osteoarthritis, which directly translates into improved mobility. The caveat is that results vary depending on preparation protocol and patient selection, which we’ll address in the next section.

WOMAC improvements are consistently reported at follow-ups of six to twelve months, with many studies showing the most meaningful gains in the three to six month window after treatment.
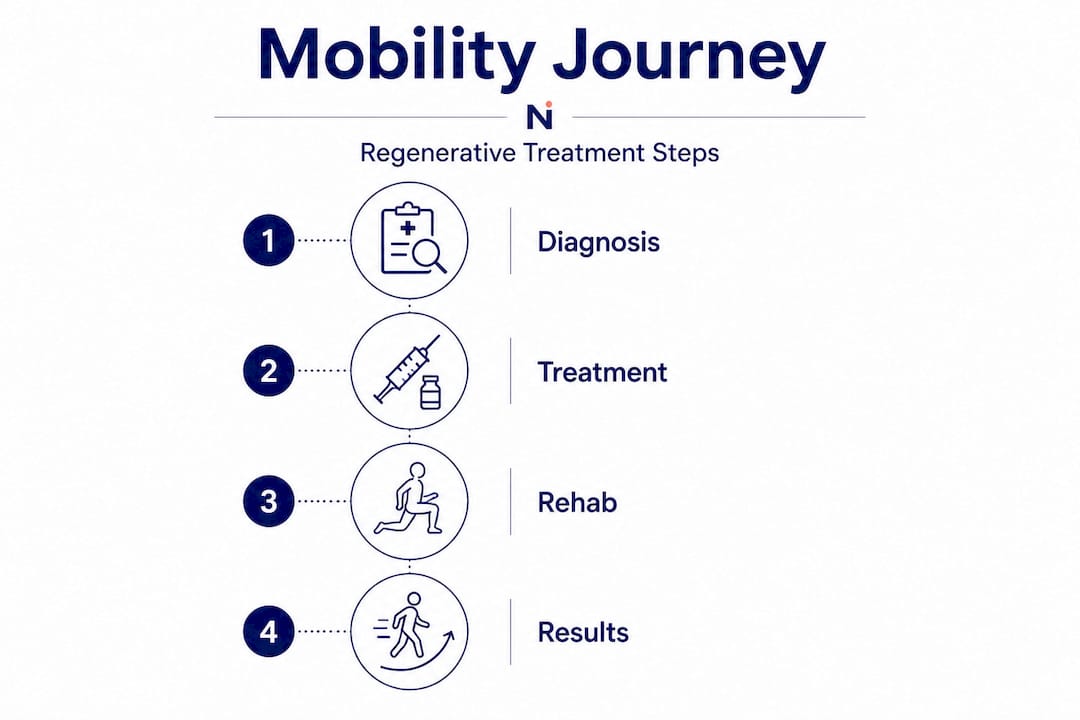
Here’s how PRP compares to two common alternatives for functional improvement:
| Treatment | Pain relief | Function improvement | Duration of benefit |
|---|---|---|---|
| PRP | Moderate to strong | Superior in most meta-analyses | 6 to 12 months |
| Hyaluronic acid | Moderate | Comparable to PRP in some studies | 3 to 6 months |
| Cortisone injection | Strong short-term | Minimal functional improvement | 4 to 8 weeks |
The data tells a clear story. Cortisone is effective for fast pain relief but offers little in the way of lasting functional improvement. Hyaluronic acid provides joint lubrication and moderate symptom relief. PRP, when properly prepared and matched to the right patient, tends to outperform both for sustained function scores, which is the measure most relevant to mobility.
Key findings active adults and athletes should understand:
- Most clinical benefit from PRP is seen in mild-to-moderate osteoarthritis, typically Kellgren-Lawrence grades I through III.
- Benefit tends to plateau or diminish in severe joint degeneration, where structural damage is too advanced.
- Multiple injections, often two to three spaced weeks apart, generally outperform single-injection protocols.
- Functional gains, including improved range of motion and reduced stiffness, are often more durable than pain relief alone.
You can explore the PRP therapy evidence behind these outcomes, and if you’re dealing specifically with knee symptoms, the detailed breakdown of PRP for knee pain is worth reading. For those managing arthritis alongside activity, PRP for arthritis covers the evidence in practical terms.
Why methodology and patient selection influence results
Even with promising results, details matter. Here’s why your individual outcome may vary, and how to stack the odds in your favor.
One of the most important things to understand about PRP is that it is not a single, standardized product. PRP preparation variability, including differences in leukocyte content, platelet concentration, activation method, injection number, and injection spacing, is a major reason trial results and guideline recommendations can differ so widely. Two patients who both receive “PRP” may actually receive very different biological products.
This variability matters because it directly affects outcomes. Leukocyte-poor PRP, for example, may be better suited for intra-articular joint injections because it produces less post-injection inflammation. Leukocyte-rich PRP may be more appropriate for tendon injuries where an inflammatory response supports healing. Getting this wrong doesn’t mean the therapy fails entirely, but it can significantly reduce the benefit you experience.
Here’s a comparison of how key protocol components affect mobility outcomes:
| Protocol variable | Lower-quality approach | Optimized approach |
|---|---|---|
| Platelet concentration | Inconsistent, not measured | Standardized, verified concentration |
| Leukocyte content | Not tailored to condition | Matched to joint vs. tendon target |
| Number of injections | Single injection only | Series of 2 to 3 injections |
| Injection spacing | Ad hoc timing | Evidence-based intervals |
| Activation method | Variable | Consistent protocol |
Beyond preparation, patient selection is equally important. PRP is generally recommended for mild-to-moderate osteoarthritis, typically Kellgren-Lawrence grades I through III, with caution in severe disease, and evidence for cartilage regeneration remains limited. This is an honest limitation that any reputable clinic should communicate clearly.
Steps to identify whether you’re a strong candidate for regenerative treatment:
- Get imaging done first. An MRI or X-ray helps determine the degree of joint degeneration and guides realistic expectations.
- Assess your activity level and goals. Athletes returning to sport have different needs than someone managing daily stiffness.
- Review your inflammatory baseline. Conditions like uncontrolled diabetes or active infection can affect healing response.
- Discuss protocol specifics with your provider. Ask about platelet concentration targets, leukocyte content, and the number of planned injections.
- Confirm your OA grade. If you’re at grade IV, a candid conversation about realistic outcomes is essential before committing.
Pro Tip: Before your first appointment, ask your provider exactly how they prepare their PRP. A clinic that can’t answer questions about platelet concentration or leukocyte content may not be following an evidence-based protocol. Comparing options? The breakdown of PRP vs prolotherapy and PRP vs cortisone can help you understand the differences clearly.
Integrating regenerative treatments with rehab and load management
Choosing the right therapy is only part of the equation. Let’s see how to get the most from your investment in joint health.
One of the most consistent findings across regenerative medicine research is that injections alone rarely deliver the best outcomes. The biology of joint repair is supported by movement, load, and structured rehabilitation. Without those elements, even a well-prepared PRP injection has a ceiling on what it can achieve.
Regenerative interventions should be integrated with load management and rehabilitation rather than treated as standalone cartilage regrowth solutions. Evidence is strongest for symptom and function improvement, while structural regeneration remains uncertain. Expectations should be framed around mobility, pain function, and disease modification rather than guaranteed tissue regrowth.
For active adults and athletes in North Texas, this means building a recovery plan that treats the injection as one tool within a broader strategy. Here’s what that looks like in practice:
- Rest appropriately after injection. Most protocols recommend avoiding high-impact activity for three to five days post-injection to allow the growth factors to work without mechanical disruption.
- Begin graded activity within the first two weeks. Light movement, including walking and gentle range-of-motion exercises, supports the healing environment without overloading the joint.
- Engage in structured physical therapy. Strengthening the muscles around the joint, particularly the quadriceps for knee OA, reduces mechanical stress on the treated area.
- Manage load progressively. Return to sport or high-demand activity should follow a graded timeline, not a fixed calendar date.
- Set realistic expectations. Mobility improvement is typically gradual. Most patients see meaningful progress between weeks six and sixteen.
- Track your progress with objective measures. Range of motion, step count, and functional tests give you concrete data to assess improvement over time.
Clinical reminder: The goal of regenerative treatment is to improve your quality of movement and reduce the pain that limits it. It is not a guarantee of structural cartilage regrowth. Patients who understand this distinction tend to report higher satisfaction because they measure success accurately.
For athletes specifically, combining regenerative treatment with physical therapy has shown strong results in the literature. The detailed approach to combining PRP and physical therapy outlines how to structure that integration effectively.
What most guides miss about regenerative mobility treatments
Most articles on regenerative medicine focus on what these treatments can do. Fewer are honest about the gap between what patients hope for and what the evidence actually supports. That gap matters, and we think you deserve a clear-eyed view.
The most common overpromise in this space is cartilage regrowth. Patients come in hoping that PRP or stem cells will rebuild the cartilage they’ve lost over years of activity and wear. The reality is more nuanced. Many regenerative studies are short-to-mid follow-up in duration and report patient-reported outcomes. Durable effects and structural outcomes, including cartilage thickness and integrity, remain harder to confirm consistently, which contributes to cautious guideline positions.
That said, we believe the more realistic win is genuinely valuable. Improved pain scores, better range of motion, reduced stiffness in the morning, and the ability to return to the activities you love, these are meaningful outcomes. For a runner who hasn’t completed a 5K in two years because of knee pain, getting back on the trail is a real, life-changing result. It doesn’t require cartilage regrowth to matter.
What we’ve seen consistently is that patients who engage in comprehensive care, including rehab, lifestyle modification, and realistic goal-setting, achieve better and more lasting outcomes than those who treat the injection as a shortcut. The biology supports this. Joint health is influenced by body weight, muscle strength, activity patterns, sleep, and systemic inflammation. A PRP injection can shift the joint environment toward repair, but it cannot override the factors that created the problem in the first place.
The most durable mobility gains come from patients who treat regenerative therapy as a catalyst, not a cure. They use the reduction in pain as a window to build strength, improve movement patterns, and address the lifestyle factors that contributed to joint stress. That’s the approach we advocate for every patient we see, and it’s the one most supported by the evidence. If you’re curious about the broader role of PRP for chronic pain, the research is encouraging when treatment is framed correctly.
Explore advanced regenerative therapy options in North Texas
If you’re an active adult or athlete in North Texas dealing with joint pain, stiffness, or a sports injury that’s limiting your movement, Nortex Tissue Regeneration offers evidence-based regenerative protocols designed around your specific condition and goals. We don’t offer one-size-fits-all injections. We build personalized treatment plans that account for your joint health, activity level, and recovery timeline.
Our team specializes in PRP therapy, stem cell therapy, and bone marrow cell therapy, each tailored to the severity and nature of your condition. Whether you’re managing early-stage osteoarthritis or recovering from a sports injury, we’re here to help you move better, hurt less, and stay active. Reach out to schedule a consultation and find out which approach fits your situation best.
Frequently asked questions
How long does it take to see improved mobility after regenerative treatments?
Most patients notice meaningful improvements in pain and function within six to twelve months, with the greatest gains typically seen in the three to six month window after treatment.
Are regenerative treatments suitable for severe joint degeneration?
PRP and similar therapies are primarily recommended for mild-to-moderate osteoarthritis, typically Kellgren-Lawrence grades I through III. Effectiveness for severe cases remains uncertain and should be discussed honestly with your provider.
Can regenerative treatments fully restore cartilage?
Current evidence shows limited cartilage regeneration from PRP and similar therapies. The more consistent and clinically meaningful outcomes are improvements in pain and functional mobility rather than structural cartilage restoration.
What’s the difference between PRP and stem cell therapy for mobility?
PRP uses concentrated platelets from your own blood to deliver growth factors that stimulate local healing, while stem cell therapy aims to introduce cells that may promote more substantial tissue regeneration. Both target pain and mobility but work through distinct biological mechanisms and are suited to different conditions and severity levels.
Does insurance cover regenerative treatments for mobility issues?
Most regenerative treatments, including PRP and stem cell injections, are not covered by insurance and are classified as elective or investigational by most health plans. Your provider can discuss financing options and help you understand the full cost before you commit.
Recommended
- Step-by-step stem cell treatment guide for joint recovery
- How stem cells heal joints: Evidence and real answers
- How Does PRP Compare to Prolotherapy for Joint Healing? – Nortex Tissue Regeneration
- Texas Tissue Regeneration – Nortex Tissue Regeneration
- Top 5 Reasons Mobility and Recovery are Crucial for Active Lifestyles
- Nonsurgical Options for Tendon and Ligament Injuries – Stride Foot & Ankle – Dr. Nahad Wassel