If you’re an active adult or athlete in North Texas dealing with persistent knee pain, a nagging tendon injury, or early arthritis, you’ve probably heard terms like PRP, stem cells, prolotherapy, and exosomes thrown around with equal enthusiasm and equal vagueness. The most commonly discussed orthobiologic injectable therapies for musculoskeletal joint pain include platelet-rich plasma, prolotherapy, autologous mesenchymal stem cells, and human-derived allograft products, yet most patients receive little guidance on how these options actually differ. This article breaks down each therapy clearly, compares them side by side, and gives you the practical criteria to ask smarter questions before committing to any treatment.
Table of Contents
- How to evaluate regenerative medicine options
- Platelet-rich plasma (PRP): How it works for joints and injuries
- Stem cell and cell-derived therapies: Potential and pitfalls
- Prolotherapy and other injectables: What to know
- Comparison of regenerative medicine treatments for joint pain
- Our take: What matters most when choosing regenerative medicine
- Explore your regenerative medicine options in North Texas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Compare by preparation | The way PRP, stem cells, and other biologics are made affects results as much as the type of therapy itself. |
| Evidence varies between therapies | PRP and some cell-based injections have more research support than newer or alternative options like exosomes or prolotherapy. |
| Ask about protocols | Always check how a treatment is prepared, activated, and dosed, as this directly impacts effectiveness and safety. |
| Not all clinics are equal | Find clinics that prioritize evidence, transparency, and fully integrate rehab for the best chance of success. |
How to evaluate regenerative medicine options
Not all regenerative therapies are created equal, and the label on a treatment rarely tells the full story. Before you compare specific options, it helps to understand what actually separates a high-quality protocol from a mediocre one.
Here are the core criteria worth examining for any regenerative injectable:
- Source material: Is the biologic derived from your own blood, your own tissue, a donor, or a lab-processed product?
- Preparation method: How is the material processed? Is it centrifuged, filtered, or expanded in a lab?
- Activation strategy: Is PRP activated with calcium chloride, thrombin, or left unactivated? Does the protocol specify this?
- Dosing: How much is injected, and how many sessions are planned?
- Rehab integration: Is physical therapy or structured activity built into the recovery plan?
- Transparency: Does the clinic explain leukocyte content, platelet concentration, or cell viability?
Preparation and activation heterogeneity across PRP and stem cell injections is a major nuance for athletes and active adults, because it limits reproducibility and makes direct comparisons between studies, and between clinics, genuinely difficult. Two patients receiving “PRP” at different facilities may be getting very different products. Understanding why PRP results vary between providers is one of the most important steps you can take before choosing a clinic.
Direct-to-consumer marketing often glosses over these details. A clinic that can’t explain their preparation protocol in plain language is a clinic worth reconsidering.
Pro Tip: Ask any regenerative medicine provider to describe their specific preparation protocol, including platelet concentration targets and whether the injection is image-guided. A confident, detailed answer is a strong sign of clinical rigor.
Platelet-rich plasma (PRP): How it works for joints and injuries
PRP is the most established and most studied of the regenerative injectables currently used in orthopedic and sports medicine settings. The process is straightforward: a small amount of your blood is drawn, placed in a centrifuge to concentrate the platelets, and then injected directly into the damaged tissue or joint.
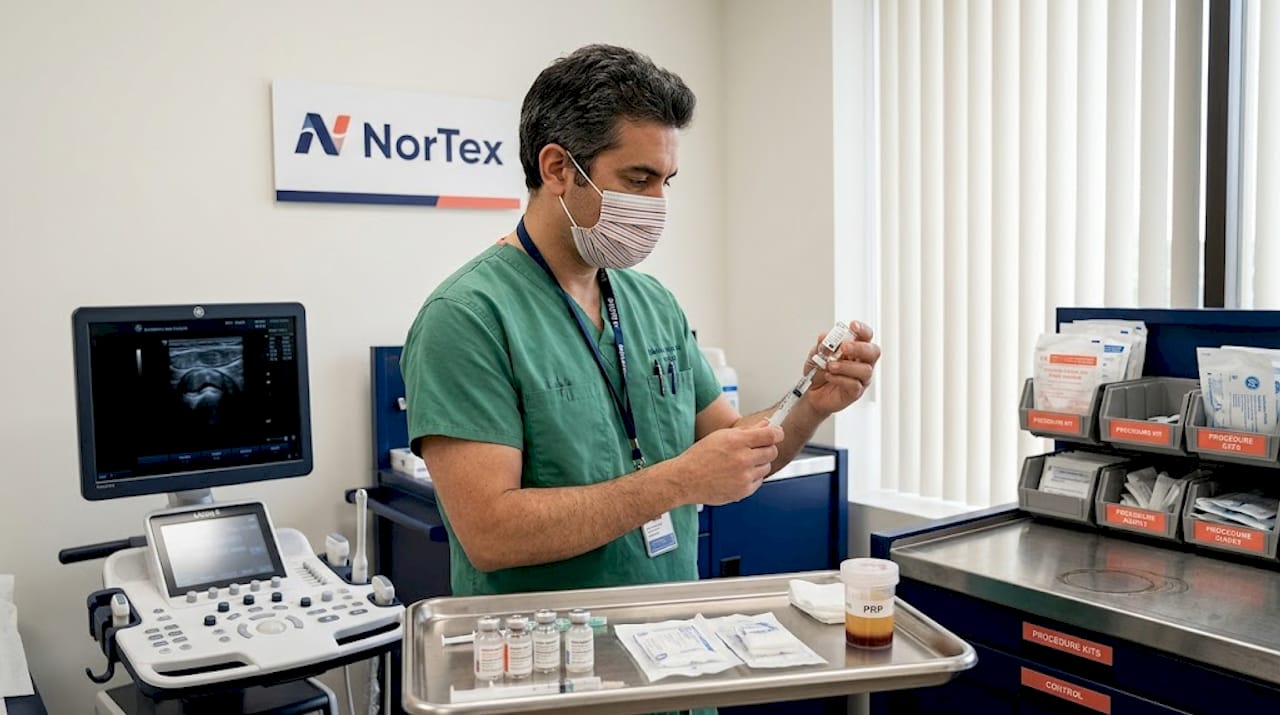
What makes PRP useful is what platelets carry. Platelet concentrates deliver growth factors and signaling molecules into damaged tissue, which may reduce inflammation and support the body’s natural repair process. These growth factors include PDGF, TGF-beta, VEGF, and IGF-1, each playing a role in tissue remodeling and pain modulation.
PRP is most commonly used for:
- Knee osteoarthritis: One of the most studied applications, with multiple trials showing meaningful symptom improvement over hyaluronic acid injections.
- Tendon injuries: Including patellar tendinopathy, Achilles tendinopathy, and lateral epicondylitis (tennis elbow).
- Muscle strains and partial tears: Particularly in athletes who need to return to activity faster.
- Rotator cuff conditions: As a conservative option before considering surgery.
- Hip labral irritation: Used as part of a broader management plan.
The evidence for PRP is strongest in knee osteoarthritis and certain tendon conditions. However, outcomes depend heavily on protocol. Leukocyte-rich versus leukocyte-poor PRP, for example, appears to produce different results depending on the condition being treated. For joint inflammation, leukocyte-poor preparations may be preferable. For tendon healing, leukocyte-rich formulations may offer an advantage.
You can read more about PRP therapy details and explore whether PRP for knee pain aligns with your specific situation.
Pro Tip: If a clinic offers PRP but doesn’t mention leukocyte content or platelet concentration, ask directly. These details matter for matching the right PRP formulation to your specific condition.
Stem cell and cell-derived therapies: Potential and pitfalls
Stem cell therapy generates significant excitement, and for good reason. The theoretical potential is real. But the gap between what’s scientifically established and what’s being marketed to patients is wider than most people realize.
There are several categories of stem cell and cell-derived therapies currently available or being studied:
- Autologous MSCs (mesenchymal stem cells): Harvested from your own bone marrow or fat tissue, then injected into the affected area. These cells have anti-inflammatory and potentially regenerative properties.
- Donor allograft products: Derived from donated tissue such as amniotic membrane, umbilical cord, or placental tissue. These are processed and sold commercially. Their actual stem cell content is often low or absent after processing.
- Exosomes and extracellular vesicles (EVs): Cell-free products derived from stem cells or platelets. Preclinical research on exosomes explores anti-inflammatory and regenerative mechanisms, but human clinical data remains limited.
The critical issue here is regulatory oversight. The FDA approves stem cells only for specific medical indications, primarily blood-related conditions. Many stem cell offerings marketed directly to consumers are unproven and may not meet FDA standards for safety or efficacy. This doesn’t mean all stem cell treatments are ineffective. It means you need to ask hard questions and verify that the clinic is operating within a clear evidence-based or trial-based framework.
Statistic callout: A significant proportion of stem cell clinics marketing orthopedic treatments in the United States operate outside of FDA-approved clinical trial frameworks, meaning their outcomes are not systematically tracked or reported.
Exosome therapies are particularly interesting from a research standpoint, but they sit firmly in the early-adopter category. If a clinic is offering exosome injections as a standard treatment, ask what clinical trial data supports their specific product and protocol. Enthusiasm for a mechanism is not the same as evidence for an outcome.
For a balanced overview of what’s currently available, our stem cell therapy overview explains how we approach these options at Nortex Tissue Regeneration.
Prolotherapy and other injectables: What to know
Prolotherapy is one of the older regenerative injection techniques, and it often gets overlooked in conversations dominated by PRP and stem cells. It deserves a fair assessment.
Prolotherapy typically involves injecting a sugar solution, usually dextrose, sometimes combined with saline or a local anesthetic, into ligaments, tendons, or joint spaces. The goal is to create a mild inflammatory response that triggers the body’s natural healing cascade. It’s a lower-tech approach, but that doesn’t make it without value.
Key points about prolotherapy and related injectables:
- Mechanism: Controlled irritation of tissue to stimulate collagen production and local healing.
- Common uses: Chronic low back pain, knee ligament laxity, shoulder instability, sacroiliac joint pain.
- Evidence profile: Evidence for prolotherapy and saline is highly condition-dependent, with some positive data for low back pain and knee osteoarthritis, but less consistency across other applications.
- Risk profile: Generally low-risk when performed correctly. No biologic material means fewer concerns about immune response or regulatory issues.
- Cost: Often more accessible than PRP or stem cell therapies.
Prolotherapy occupies a practical middle ground in regenerative care. It’s not the most powerful tool available, but for patients who aren’t candidates for PRP, or who want to start with a lower-risk option, it offers a reasonable entry point into biologic-style care.
Prolotherapy is sometimes used as part of a multimodal approach, combined with PRP or physical therapy, rather than as a standalone treatment. If you’re weighing your options, it’s worth understanding how PRP compares to prolotherapy for joint healing before making a decision.
Comparison of regenerative medicine treatments for joint pain
To help you see the differences clearly, here’s a direct comparison of the major regenerative medicine options for joint pain and musculoskeletal injuries. Keep in mind that evidence for specific products remains incomplete and requires further standardization across the field.
| Therapy | Source | Preparation | Evidence strength | Best-fit conditions | Key considerations |
|---|---|---|---|---|---|
| PRP | Your own blood | Centrifuged, concentrated | Moderate to strong | Knee OA, tendinopathy, muscle injuries | Protocol variation affects outcomes |
| Autologous MSCs | Your own bone marrow or fat | Processed, sometimes expanded | Moderate, growing | Cartilage defects, early arthritis | Requires aspiration procedure; FDA oversight varies |
| Donor allograft products | Donated tissue (cord, amniotic) | Commercially processed | Limited to moderate | Marketed broadly, evidence mixed | Actual cell content often low after processing |
| Exosomes/EVs | Stem cells or platelets | Lab-derived, cell-free | Early/preclinical | Experimental use | Strong mechanism theory, limited human trials |
| Prolotherapy | Dextrose/saline solution | No biologic processing | Low to moderate | Ligament laxity, low back pain, knee OA | Lower risk, lower potency than PRP |
| Saline injections | Sterile saline | None | Variable (placebo-controlled trials show some benefit) | Used as comparator; occasional clinical use | Mechanism unclear; may have mechanical effect |
The most common conditions treated with PRP therapy overlap significantly with those where stem cell and prolotherapy options are also used, which is exactly why a personalized consultation matters more than a generic recommendation.
Our take: What matters most when choosing regenerative medicine
After following the advances and, frankly, the missteps in regenerative medicine over many years, we’ve developed a clear perspective that we think every patient deserves to hear.
The name of a treatment is almost irrelevant. What actually drives outcomes is the biological detail underneath the label. Biologic characterization matters, including leukocyte content, activation strategy, cell expansion methods, dosing volume, and how rehabilitation is integrated into the recovery plan. Two clinics offering the same treatment name can produce dramatically different results because their protocols differ in every meaningful way.
We’ve also seen how direct-to-consumer marketing can mislead patients who are genuinely suffering and looking for answers. Ads that promise “stem cell therapy” for any joint condition without specifying the source, the processing method, or the regulatory status of the product are not being honest with you. Enthusiasm is not evidence. A compelling before-and-after story is not a clinical trial.
Our honest advice is this: don’t choose a therapy. Choose a protocol. Ask the clinic to explain exactly what they’re injecting, how it was prepared, what concentration or cell count they’re targeting, and how they’ll support your recovery afterward. If they can’t answer those questions clearly, that tells you something important.
We’re also cautious about early adoption of exosome products and unverified allograft offerings. The science is genuinely exciting, but excitement about a mechanism doesn’t mean the product you’re being offered actually delivers that mechanism at therapeutic levels. Waiting for stronger human clinical data is not pessimism. It’s good medicine.
For patients who want to understand why some PRP treatments work better than others, the answer almost always comes back to protocol specifics, not the therapy category itself.
Explore your regenerative medicine options in North Texas
If you’re ready to move past confusion and into a clear, personalized plan, Nortex Tissue Regeneration is here to help. We offer evidence-based platelet-rich plasma therapy, stem cell therapy, and bone marrow cell therapy for active adults and athletes dealing with joint pain, sports injuries, and degenerative conditions. Our team takes the time to explain exactly what we’re recommending and why, because we believe informed patients get better outcomes. Whether you’re managing knee osteoarthritis, recovering from a tendon injury, or exploring your options before considering surgery, we’ll help you find the right path forward.
Frequently asked questions
What is the safest type of regenerative medicine for joint pain?
PRP and prolotherapy are well-established and considered safe for most adults when performed by skilled providers, while stem cell and exosome therapies require more caution given the evolving evidence base. Your provider should review your health history and condition before recommending any injectable.
How do I know if PRP or stem cell therapy is right for me?
Careful patient selection is essential to optimizing outcomes, so a specialist should review your diagnosis, activity goals, and treatment history before making a recommendation. There is no universal answer because the right choice depends on your specific condition and how far it has progressed.
Are all stem cell treatments for joint pain FDA-approved?
No. The FDA approves stem cells only for certain medical indications and actively warns consumers about unproven stem cell clinic offerings. Always ask whether the treatment you’re considering falls within an FDA-approved or supervised clinical trial framework.
What are the main risks or downsides of regenerative medicine injections?
Risks include local infection, temporary soreness, and inflammatory flare-ups, and for unproven stem cell therapies, there is a real chance of no benefit alongside potential safety concerns. Working with a transparent, medically supervised clinic significantly reduces these risks.
Recommended
- How Does PRP Compare to Prolotherapy for Joint Healing? – Nortex Tissue Regeneration
- PRP vs Cortisone Shots: Which One Is Better for Joint Pain Relief? – Nortex Tissue Regeneration
- PRP vs Stem Cell Therapy: Which One Makes Sense for You? – Nortex Tissue Regeneration
- PRP vs Cortisone: Which Injection Is Better for Joint Pain? – Nortex Tissue Regeneration