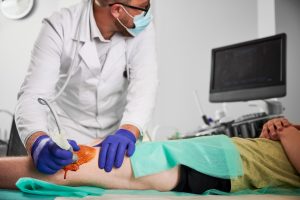
Joint pain doesn’t have to end in an operating room. For many active adults in North Texas, outpatient orthobiologics represent a genuinely different path: minimally invasive, office-based procedures that use biological materials to support tissue repair and symptom relief without hospital admission or lengthy recovery. These aren’t experimental gimmicks or marketing buzzwords. They’re a growing field backed by clinical research, used by orthopedic specialists across the country. This article walks you through what the therapies involve, what the evidence actually says, and how to make a genuinely informed decision about your own care.
Table of Contents
- What is outpatient regenerative therapy?
- How do regenerative therapies work?
- What does the evidence show for common therapies?
- Measuring success: What improvement looks like
- Choosing the right outpatient regenerative therapy clinic
- Our perspective: What actually matters for North Texas adults considering regenerative therapy
- Explore your options with Nortex Tissue Regeneration
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Minimally invasive care | Outpatient regenerative therapies use your body’s own materials for joint repair without hospital surgery. |
| Evidence varies by treatment | Some therapies like PRP show pain and function benefit, but long-term results and protocols vary widely. |
| Meaningful progress measured | Success is best tracked by pain and function improvements that meet clinical thresholds. |
| Personalization is essential | The best results come from matching therapy type to your diagnosis with an experienced clinic. |
What is outpatient regenerative therapy?
Outpatient regenerative therapy covers a category of treatments designed to support your body’s natural repair processes, primarily through injections delivered in a clinic setting. No surgical incisions. No general anesthesia. No hospital stays. You arrive, receive treatment, and typically return home the same day.
The word “outpatient” matters here. It separates these procedures from surgery not just logistically but philosophically. Surgery repairs or replaces damaged structures through direct mechanical intervention. Regenerative therapy works differently, by introducing biological materials into the affected area to modify the local environment, reduce inflammation, improve lubrication, or support cellular activity.
Common options include:
- PRP (platelet-rich plasma): Your blood is drawn, processed to concentrate growth factors and platelets, and injected into the affected joint or tissue.
- Prolotherapy: A dextrose solution is injected to stimulate a mild healing response in weakened connective tissue.
- Viscosupplementation: Hyaluronic acid is injected into joints (most often the knee) to restore lubrication and cushioning.
- Cell-based treatments: Bone marrow concentrate or adipose-derived cells are used to deliver biologic activity to the damaged area.
Here’s a quick comparison to help frame the difference between outpatient and surgical approaches:
| Feature | Outpatient regenerative therapy | Surgical intervention |
|---|---|---|
| Procedure location | Clinic or office | Hospital or surgical center |
| Anesthesia | Local or none | General or regional |
| Recovery time | Days to weeks | Weeks to months |
| Mechanism | Biologic environment modification | Structural repair or replacement |
| Insurance coverage | Often limited or out-of-pocket | More commonly covered |
| Repeat treatments | Common | Rarely repeated |
“These procedures use biological materials to support tissue repair and symptom relief, commonly via injections rather than surgery.” This distinction shapes everything from how you prepare to what you can reasonably expect.
The most important thing to understand is that outpatient regenerative therapies are not designed to instantly rebuild cartilage or reattach torn tendons the way surgery can. Their goal is to create a biological environment where your tissue has a better opportunity to heal and function. That’s a meaningful distinction when setting expectations.
How do regenerative therapies work?
Once you understand what these treatments are, the next logical question is how they act inside your body. The answer is less dramatic than you might expect, and more sophisticated.
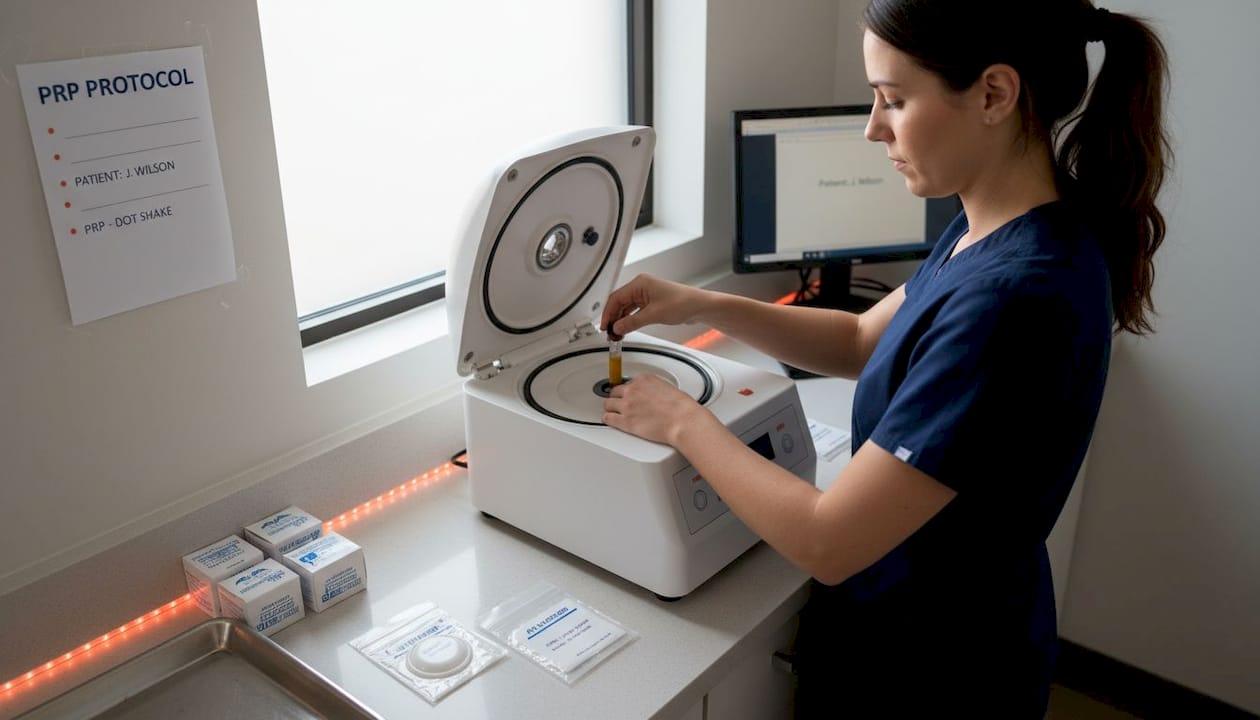
Rather than reconstructing anatomy, regenerative therapies modify the joint environment, targeting factors like inflammation, lubrication, and cellular signaling. Think of a knee with osteoarthritis. The cartilage has thinned, the synovial fluid has degraded, and the inflammatory cycle keeps the joint irritated. Regenerative therapies aim to interrupt or slow that process using the body’s own biological signals.
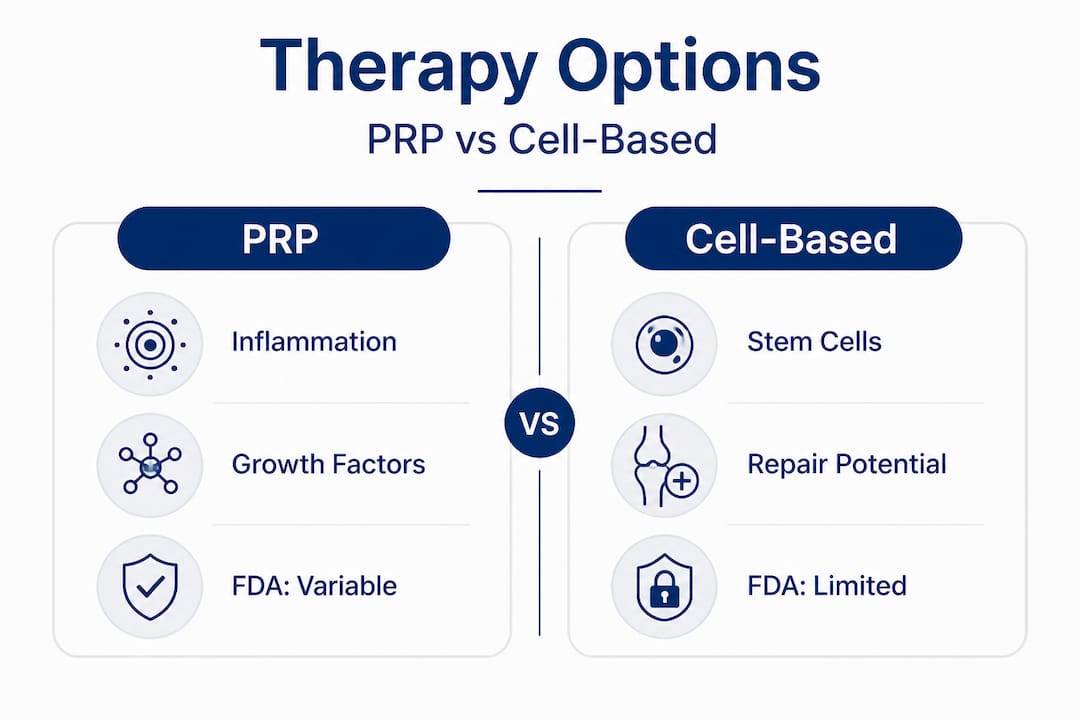
Here’s how the most common therapies work at a mechanistic level:
| Therapy | Primary target | Regulatory status |
|---|---|---|
| PRP (platelet-rich plasma) | Inflammation modulation, growth factor delivery | Investigational / off-label for most uses |
| Hyaluronic acid injections | Joint lubrication, cushioning | FDA cleared for knee osteoarthritis |
| Bone marrow concentrate | Cell-based activity, anti-inflammatory signaling | Investigational |
| Adipose-derived cells | Cellular support, inflammation reduction | Investigational |
One important clarification worth stating clearly: FDA clearance varies across these therapies. Hyaluronic acid viscosupplementation for knee osteoarthritis has specific FDA clearance. Many other biologic therapies, including PRP and most cell-based treatments, are considered investigational or used off-label. That doesn’t mean they’re unsafe or ineffective. It means the regulatory process for biologics is complex, and the evidence base is still evolving. A trustworthy clinic will explain this to you directly rather than glossing over it.
Pro Tip: Before your first appointment, ask specifically whether the therapy being recommended for your condition has FDA clearance or is being used investigationally. This question alone tells you a lot about how transparent a provider is.
For a direct comparison of two of the most discussed options, you can explore PRP vs stem cell therapy to understand how their mechanisms and indications differ in practice.
What does the evidence show for common therapies?
Understanding how treatments work leads naturally to the harder question: do they actually help? The honest answer is nuanced, and it’s worth understanding why.
For knee osteoarthritis specifically, PRP has demonstrated evidence of benefit on pain and function in clinical trials. A systematic review and meta-analysis of randomized controlled trials found PRP can offer pain relief comparable to hyaluronic acid and in some comparisons shows superior functional improvement. That’s meaningful. But the same body of research also reveals that outcomes depend heavily on patient selection, PRP formulation, preparation protocol, concentration of platelets, and dosing frequency.
Key factors that influence outcomes include:
- Diagnosis specificity: PRP performs differently for mild versus advanced osteoarthritis, and differently again for tendinopathy or ligament injuries.
- PRP formulation: The concentration of platelets and presence or absence of leukocytes (white blood cells) affects how the treatment behaves in tissue.
- Number of injections: Single injection versus multi-injection protocols produce different response patterns.
- Patient age and activity level: Younger, more active patients with less severe joint degeneration tend to respond more favorably.
- Concurrent rehabilitation: Pairing regenerative treatment with physical therapy consistently improves outcomes compared to injection alone.
Some high-quality, placebo-controlled trials show inconsistent long-term benefits, especially after 6 to 12 months. This is not a reason to dismiss these therapies. It’s a reason to be informed about what they can and cannot do for your specific situation.
Cell-based treatments, including bone marrow concentrate, carry a smaller and more variable evidence base. Early studies and real-world case series report promising pain reduction and functional improvement, but large-scale randomized trials are still limited. The field is moving quickly, and what was investigational five years ago is increasingly supported by emerging data.
Pro Tip: Not all PRP is the same. Ask your provider what platelet concentration they target, whether their protocol is leukocyte-rich or leukocyte-poor, and how many injections are planned. These specifics shape your result far more than the brand name of the treatment.
For condition-specific information, you can read more about PRP for arthritis and knee pain and explore PRP as a surgical alternative. It’s also worth understanding how PRP compares to prolotherapy if you’re evaluating multiple options.
Measuring success: What improvement looks like
Knowing the evidence exists is one thing. Knowing what improvement actually feels like, and how to measure it, is something most patients never get explained to them clearly.
Clinicians use specific benchmarks called MCID (Minimal Clinically Important Difference) and SCB (Substantial Clinical Benefit) to determine whether a treatment produced meaningful change in a patient’s pain or function scores. These are thresholds that go beyond statistical significance. They ask: did the patient notice a real difference in their daily life?
In one study of knee osteoarthritis treated with combination autologous orthobiologics, high rates of patients met MCID and SCB thresholds at 12 months, with 87% reaching clinically meaningful improvement and 59% achieving substantial benefit. Those are meaningful numbers for a patient population that often feels like they’ve run out of options.
Here’s how to use this framework practically during your own recovery:
- Establish a baseline. Before treatment, document your pain level on a 0 to 10 scale and note specific functional limitations, such as how far you can walk, whether you can climb stairs without discomfort, or what activities you’ve had to modify.
- Track at regular intervals. At 6 weeks, 3 months, 6 months, and 12 months, revisit those same measures. Improvement often comes gradually, and without a baseline, it’s easy to underestimate progress.
- Use validated tools. Ask your provider about outcome measures such as the KOOS (Knee Injury and Osteoarthritis Outcome Score) or WOMAC. These patient-reported tools are what research studies use, and applying them to your own case gives you data, not just feelings.
- Communicate changes clearly. If your improvement stalls or reverses, tell your provider early. Catching a plateau at 3 months allows for protocol adjustment before 6 months pass with no progress.
Pro Tip: Keep a simple recovery journal. A few sentences per week about what you could and couldn’t do is more useful in a follow-up appointment than trying to remember how you felt months ago. It also helps your provider make smarter adjustments to your plan.
Choosing the right outpatient regenerative therapy clinic
Once you understand what meaningful improvement looks like, you’re in a much better position to evaluate the clinics and providers in your area. Matching the underlying diagnosis to the specific biologic and its evidence base is the most practical framework for comparing your options.
Before committing to a clinic or treatment plan, ask these specific questions:
- What is my specific diagnosis, and what evidence exists for this therapy with that diagnosis? General claims about regenerative medicine are not enough. You want condition-specific data.
- Is this treatment FDA cleared for my indication, or is it investigational? Both can be valid, but you deserve an honest answer upfront.
- Who performs the injection, and what training do they have in image-guided procedures? Ultrasound guidance significantly improves placement accuracy, especially for smaller joints and tendons.
- How do you measure outcomes for your patients? Clinics using standardized outcome tools are generally more rigorous in their protocols.
- What does the full treatment plan look like? One injection is rarely the whole story. Understand the planned number of sessions, the expected timeline, and what rehabilitation is recommended alongside treatment.
- What happens if I don’t respond? A good provider has a clear plan for non-responders and doesn’t overpromise.
Understanding why PRP results vary between patients and clinics is also valuable context as you evaluate your options. The difference between a well-executed and a poorly executed protocol can be significant.
Our perspective: What actually matters for North Texas adults considering regenerative therapy
We work with active adults every day who come in carrying a mix of hope and skepticism, and honestly, both are appropriate. Regenerative medicine has been overhyped in some corners of the internet and undersold in others. The truth sits somewhere more practical.
Here’s what we’ve observed consistently: the single biggest predictor of a good outcome isn’t the therapy itself. It’s the match between the diagnosis and the treatment. A patient with mild to moderate knee osteoarthritis and a well-executed PRP protocol has a genuinely strong chance of meaningful improvement. That same therapy applied to advanced joint degeneration with significant structural loss will likely disappoint, not because PRP doesn’t work, but because the biology of the situation is different.
Most online content about regenerative medicine skips this distinction entirely. It presents these therapies as broadly effective, almost universally beneficial, which does patients a real disservice. It sets expectations that can’t be met and leaves people confused when they don’t see dramatic results.
What we’d encourage you to resist is the appeal of any clinic that talks more about the therapy than about your diagnosis. The conversation should begin with what’s happening in your joint or tissue, what imaging shows, and what your functional goals are. The therapy choice comes after that assessment, not before it.
We’d also gently challenge the assumption that newer means better in this space. PRP has more published clinical trial data than most newer cell-based approaches. That doesn’t make cell-based therapy inferior, but it means the evidence base should guide conversations about realistic expectations. When choosing between PRP and stem cell therapy, that comparison should always be anchored to your specific condition and clinical profile.
Trust providers who give you conservative estimates and reference the literature. Be cautious of any clinic that promises dramatic results without acknowledging the variability in outcomes that research consistently shows.
Explore your options with Nortex Tissue Regeneration
If you’re an active adult in North Texas dealing with joint pain, a sports injury, or a degenerative condition and you’re curious about non-surgical options, Nortex Tissue Regeneration is here to help you move from information to action. We offer evidence-led, personalized treatment plans built around your specific diagnosis, not a one-size-fits-all menu.
Our services include PRP therapy with individualized protocols, bone marrow cell therapy for patients where cell-based biologics are appropriate, and stem cell therapy as part of a broader regenerative approach. Every consultation begins with a thorough clinical evaluation, and every treatment plan is tied to measurable outcomes. We believe you deserve clear, honest guidance, and we’re committed to delivering exactly that.
Frequently asked questions
What is the difference between outpatient regenerative therapy and surgery?
Outpatient regenerative therapies use injections of biological materials in a clinic setting and do not require hospital admission, while surgery involves incisions, anesthesia, and structured operative recovery. The core distinction is that regenerative therapies modify the joint environment biologically, whereas surgery addresses structural problems mechanically.
Is PRP for joint pain FDA approved?
PRP is widely used for joint pain but is generally considered investigational or off-label for most musculoskeletal indications. FDA clearance in this space is specific: hyaluronic acid viscosupplementation for knee osteoarthritis holds it, while PRP and most cell-based treatments do not for all uses.
What outcomes should I expect from regenerative joint therapy?
Most patients experience some improvement in pain and function within the first 6 to 12 months, but results vary considerably based on therapy type, protocol, and individual diagnosis. Research on PRP for knee osteoarthritis confirms that protocol heterogeneity and patient selection are major drivers of outcome variability.
How is meaningful improvement measured after outpatient regenerative therapy?
Meaningful improvement is tracked using patient-reported outcome measures that must reach or exceed established MCID and SCB thresholds to be considered clinically significant. In one study, high proportions of patients treated with combination orthobiologics met those thresholds at 12 months, providing a useful benchmark for your own recovery expectations.
Recommended
- PRP vs Stem Cell Therapy: Which Is Right for You? – Nortex Tissue Regeneration
- How stem cells heal joints: Evidence and real answers
- Why Some PRP Treatments Work Better Than Others – Nortex Tissue Regeneration
- PRP vs Stem Cell Therapy: Which One Makes Sense for You? – Nortex Tissue Regeneration
- Parent guide to gene therapy: options, risks, and what to expect
- Nonsurgical Options for Tendon and Ligament Injuries – Stride Foot & Ankle – Dr. Nahad Wassel