If you have been living with joint pain for a while, you have likely heard about PRP therapy for arthritis. We see many patients at this stage—trying to manage daily discomfort, unsure about the next step, and often hoping to avoid surgery if possible. In our experience, treatments like platelet-rich plasma (PRP) therapy can offer a different path. Not a shortcut, and not a cure, but a way to support how your body heals.
Arthritis tends to progress slowly, but steadily. The question we often work through together is not just “What reduces pain?” but “What helps you function better over time?”
Understanding Arthritis and Joint Degeneration
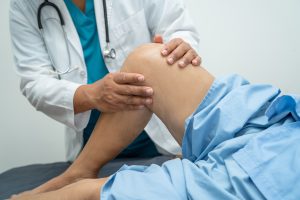
Arthritis is not a single condition. Most of the patients we see are dealing with osteoarthritis, where the joint cartilage gradually wears down. This leads to stiffness, swelling, and pain that tends to worsen with activity.
What we often notice is that by the time people consider treatment, the joint has already gone through measurable degeneration. Cartilage is thinner. Inflammation is more persistent. Movement becomes limited.
Traditional care usually focuses on symptom management:
- Anti-inflammatory medications
- Cortisone injections
- Physical therapy
These can help, especially early on. But over time, they may not address the underlying changes happening inside the joint.
Where PRP Fits In
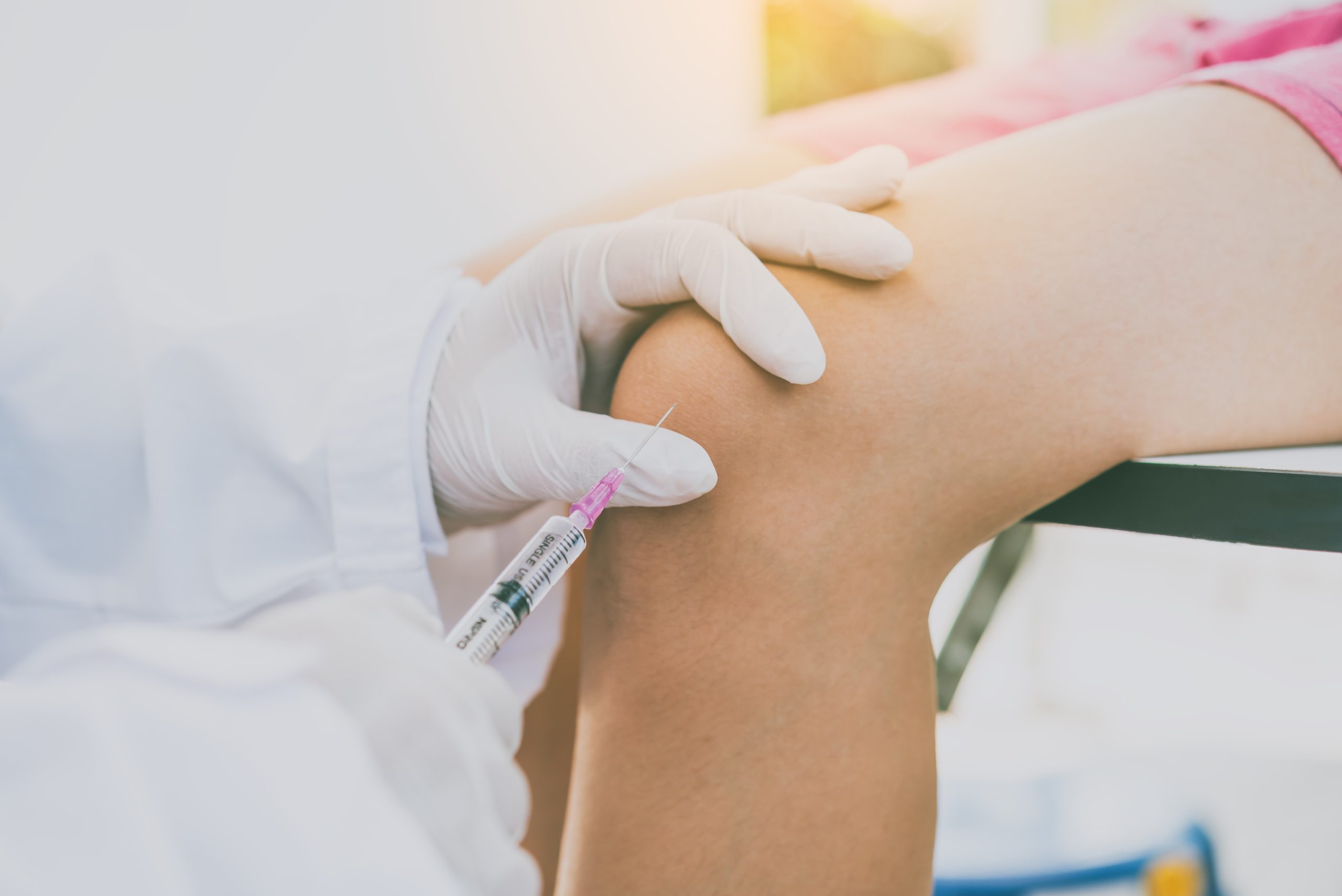
PRP stands for platelet-rich plasma. It is prepared from your own blood, concentrated to isolate platelets and growth factors, and then injected into the affected joint.
When we use PRP therapy, the goal is not to replace damaged tissue directly. Instead, it is to support the body’s natural repair response.
In our experience, PRP works best as part of a broader joint degeneration treatment approach. It can help:
- Modulate inflammation
- Support tissue repair signaling
- Improve the joint environment over time
It is a gradual process. Most people do not feel a dramatic change overnight. That is important to understand early.
PRP Therapy for Arthritis: What We Often See
When patients come in for arthritis PRP injections, they usually ask the same question: “Will this keep me from needing surgery?”
The honest answer is—it depends.
We have learned over time that PRP tends to be more effective in certain situations:
- Mild to moderate arthritis
- Patients who are still active
- Joints that have not fully deteriorated
In these cases, we often see:
- Reduced pain levels over several weeks
- Improved joint mobility
- Better tolerance for daily activity
In more advanced arthritis, PRP may still help with symptom control. But expectations need to be realistic. It may not replace the need for surgery in every case.
The Process: What Treatment Actually Looks Like
We try to keep the process straightforward.
First, we evaluate the joint carefully. Imaging, physical exam, and your symptom history all matter. Not every case of joint pain is the same, even if it feels similar.
The PRP procedure itself involves:
- Drawing a small amount of your blood
- Processing it to concentrate platelets
- Injecting it into the affected joint under guidance
The injection is usually done in a single visit. Some patients need a series of treatments, depending on how the joint responds.
Afterward, we often recommend a short period of reduced activity, followed by a gradual return to movement, sometimes paired with physical therapy.
How PRP Compares to Other Non-Surgical Options
PRP is one option among several non-surgical relief strategies. It is not always the first step.
Cortisone injections, for example, can reduce inflammation quickly. But repeated use may not support long-term joint health.
Other regenerative approaches may also be considered:
- Stem cell-based therapies
- Energy-based treatments
- Soft tissue-focused therapies
In some cases, we combine PRP with treatments like shockwave therapy to improve circulation and tissue response around the joint.
We have learned that combination approaches can sometimes produce more consistent outcomes, especially in more persistent cases.
Who Is a Good Candidate for PRP?
This is one of the most important parts of the conversation.
PRP Therapy for Arthritis is not ideal for everyone. In our experience, good candidates tend to:
- Have early to mid-stage arthritis
- Want to stay active and delay surgery
- Be willing to follow a structured recovery plan
Patients who expect immediate results or a one-time fix may feel frustrated. PRP Therapy for Arthritis requires patience.
We also look at overall health. Healing capacity varies from person to person, and that affects how well PRP works.
What Results Feel Like Over Time
The timeline with PRP is not linear.
Most patients notice subtle changes first:
- Less stiffness in the morning
- Slight improvement in movement
- Reduced flare-ups after activity
These changes often build over several weeks, sometimes months.
We have learned not to judge results too early. The body takes time to respond, especially in joints that have been inflamed for years.
Can PRP Help You Avoid Surgery?
This is the central question.
In some cases, yes. We have seen patients delay or avoid joint replacement after PRP, particularly when treatment starts early and is combined with appropriate rehabilitation.
But we are careful not to present it as a guarantee.
There are situations where surgery becomes the most practical option:
- Severe joint damage
- Persistent pain despite multiple treatments
- Significant loss of function
PRP Therapy for Arthritis can still play a role in these cases, sometimes helping manage symptoms before surgery or supporting recovery afterwards.
Looking at the Bigger Picture
Arthritis management is rarely about one treatment.
What we often see is that the best outcomes come from a combination of:
- Targeted therapies like PRP
- Strength and mobility work
- Lifestyle adjustments
We also consider other supportive treatments when appropriate, such as stem cell therapy, EMTT, or SoftWave therapy, depending on how the joint is responding.
The goal is not just pain reduction. It is helping you move better and maintain that function over time.
What We Have Learned From Treating Arthritis with PRP
Over the years, a few patterns stand out.
PRP tends to work best when:
- It is used earlier rather than later
- Patients stay consistent with rehabilitation
- Expectations are clear from the start
It is not about replacing every other treatment. It is about adding a tool that supports your body’s ability to adapt and recover.
For many patients, that is enough to change the trajectory of their joint health.
If you are considering PRP therapy for arthritis and want to understand whether it fits your situation, you can reach out to our team to talk through your options.