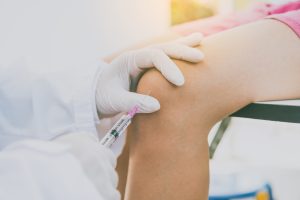
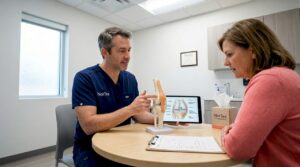
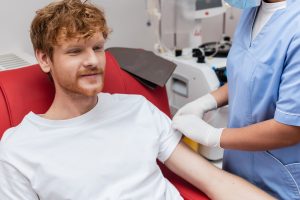
Joint pain has a way of stealing the things you love most. Whether it’s cutting your run short, skipping the weekend pickup game, or waking up stiff before a training session, chronic joint problems affect how you move and how you feel every single day. Stem cell therapy is increasingly marketed as a breakthrough non-surgical solution, and for some patients, it genuinely offers meaningful relief. But the landscape is full of bold claims that outrun the science. This guide gives you a clear, honest, step-by-step look at what stem cell treatment for joints actually involves, who it’s right for, and how to get the best possible outcome.
Table of Contents
- Understanding stem cell therapy for joints: What you need to know first
- Preparing for stem cell treatment: Who qualifies and what to expect
- Step-by-step stem cell treatment: The procedure from start to finish
- Common pitfalls and maximizing success: Dos, don’ts, and follow-up
- What most people get wrong about stem cell treatment for joint injuries
- Explore your non-surgical joint recovery options with Nortex
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Modest short-term benefits | Stem cell injections may offer slight pain and function improvement for up to six months, but with low certainty for long-term relief. |
| Not for advanced arthritis | Evidence and expert guidelines advise against routine use in severe, bone-on-bone osteoarthritis cases. |
| Match treatment to condition | Best outcomes occur when therapy targets appropriate injuries and is integrated with personalized rehab. |
| Preparation matters | Proper diagnosis, pre-procedure steps, and setting realistic expectations are key for success. |
Understanding stem cell therapy for joints: What you need to know first
Before you book a consultation, it helps to understand what stem cell therapy actually is and, just as importantly, what it is not. A stem cell therapy overview describes these treatments as biologic injections that introduce cells with the potential to reduce inflammation and support tissue repair. Unlike surgery, there are no incisions, no general anesthesia, and no lengthy hospital stay. The goal is to work with your body’s own healing mechanisms rather than replace or remove damaged tissue.
Stem cells used in joint treatments typically come from two sources: bone marrow (called bone marrow aspirate concentrate, or BMAC) and adipose tissue, which is fat harvested from your own body. Both sources contain cells and growth factors that may help calm inflammation and support the environment around damaged tissue. The key word is “may.” The science is promising but still evolving.
Here is where it gets important for active adults and athletes in North Texas. Not every joint problem responds the same way:
- Focal cartilage defects (a localized area of cartilage damage, often from a sports injury) in younger, active patients tend to show more potential for benefit.
- Early to moderate osteoarthritis may see some pain reduction and functional improvement, particularly when combined with physical therapy.
- Advanced bone-on-bone osteoarthritis is a different story. Biologic injections are not recommended for routine use in advanced hip and knee osteoarthritis due to a lack of supporting evidence.
One of the most common misconceptions is that stem cells will regrow cartilage in a worn-out joint. Current evidence does not support this for advanced cases. Another misconception is that results are permanent. In reality, stem cell injections provide only small improvements in pain and function compared to placebo, mostly up to six months, and the certainty of evidence is rated as very low.
“The goal of stem cell therapy is not to rebuild a joint from scratch. It is to reduce inflammation, support tissue health, and improve function in the right patient at the right stage of their condition.”
Understanding this sets realistic expectations, which is the foundation of a successful treatment experience.
Preparing for stem cell treatment: Who qualifies and what to expect
Knowing whether you are a good candidate is the single most important step before pursuing treatment. Not everyone with joint pain will benefit, and going in without the right evaluation is one of the most common reasons patients feel disappointed with results.
Basic eligibility factors that providers typically assess include:
- Age and overall health: Younger patients with strong baseline health tend to have more robust healing responses.
- Type and severity of joint damage: Focal injuries and early to moderate arthritis are generally more responsive. Candidates with advanced bone-on-bone arthritis are generally not ideal; earlier stage or focal defects may benefit more depending on cell type and rehabilitation.
- Activity level and goals: Athletes and active adults who are committed to post-treatment rehab tend to achieve better outcomes than those who expect passive recovery.
- Prior treatment history: If you have already tried physical therapy, anti-inflammatory medications, or PRP injections, your provider will factor that into the evaluation.
What to bring to your consultation:
| Item | Why it matters |
|---|---|
| Imaging (X-ray, MRI) | Shows the extent of joint damage and guides treatment planning |
| List of current medications | Some medications affect healing and cell function |
| Pain and activity history | Helps establish baseline and set realistic goals |
| Prior treatment records | Avoids redundant steps and informs next best options |
| Insurance documentation | Most stem cell injections are not covered; knowing costs upfront matters |
Before your visit, you will likely need updated imaging. X-rays show bone structure and joint spacing, while MRI gives a clearer picture of soft tissue, cartilage, and ligament health. Your provider may also conduct a physical exam to assess range of motion, swelling, and functional limitations.

If you are unsure whether this treatment is right for your situation, you can find out if you’re a candidate through a personalized evaluation. It is also worth exploring how PRP vs stem cell therapy compares, since PRP (platelet-rich plasma) is often a complementary or alternative option depending on your diagnosis.
Pro Tip: Start keeping a daily pain and activity log at least two weeks before your consultation. Note your pain level on a 1 to 10 scale, what activities triggered or relieved it, and how it affected your sleep and performance. This gives your provider concrete data and helps you track progress after treatment.
Step-by-step stem cell treatment: The procedure from start to finish
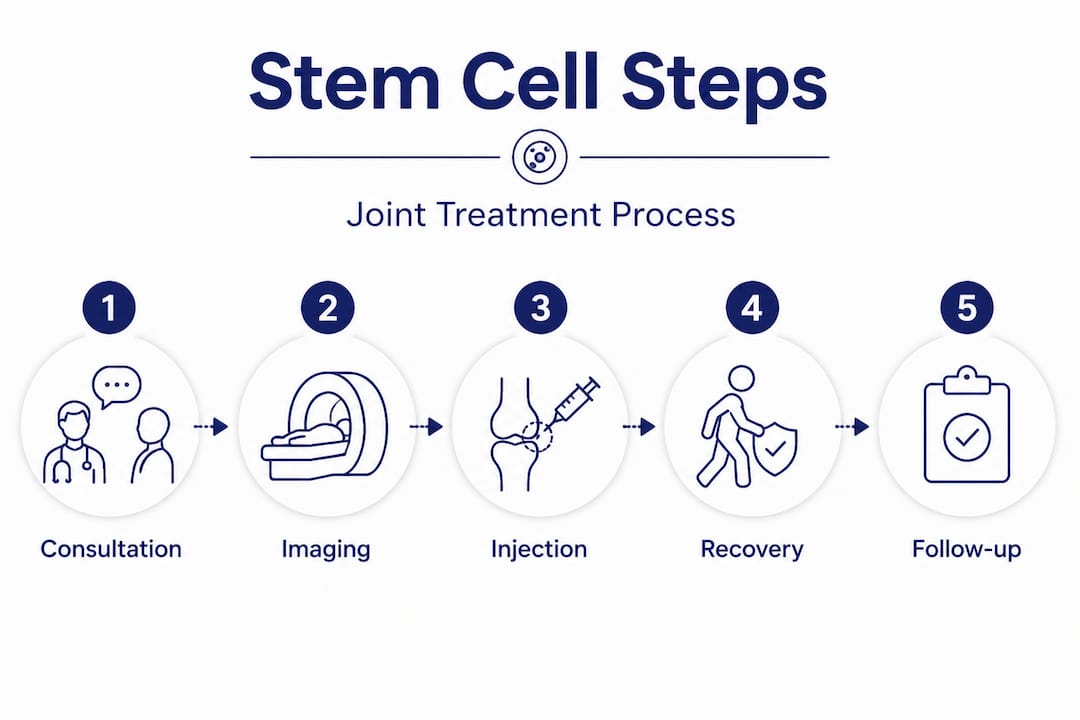
Understanding exactly what happens on treatment day reduces anxiety and helps you prepare properly. Here is what a standard same-day stem cell injection procedure looks like:
- Pre-procedure preparation: You will arrive at the clinic having followed specific instructions, which typically include avoiding anti-inflammatory medications (like ibuprofen) for one to two weeks before treatment, since these can interfere with cell activity.
- Harvesting: If bone marrow is used, a small amount is drawn from the back of your hip bone using a needle under local anesthesia. If fat-derived cells are used, a mini liposuction procedure collects a small amount of adipose tissue from your abdomen or flank.
- Processing: The harvested material is placed in a centrifuge, a machine that spins rapidly to concentrate the stem cells and growth factors. This takes roughly 15 to 30 minutes.
- Ultrasound-guided injection: Using real-time imaging, the provider injects the concentrated cells directly into the affected joint. Ultrasound guidance improves precision and accuracy significantly.
- Aftercare and observation: You rest briefly at the clinic, then receive detailed aftercare instructions before heading home.
Comparing treatment types:
| Treatment type | Invasiveness | FDA approval | Recovery time |
|---|---|---|---|
| Same-day BMAC or fat-derived injection | Minimally invasive, office-based | Not FDA approved for joints | Days to weeks |
| MACI (cartilage implant) | Surgical | FDA approved for specific knee defects | Months |
| PRP injection | Minimally invasive, office-based | Not FDA approved | Days |
It is important to understand this distinction clearly. Most marketed stem cell treatments are same-day procedures using bone marrow or fat-derived cells. Cultured cell implants like MACI involve surgery and are FDA approved only for specific knee cartilage defects in younger patients. Standard office-based injections do not carry FDA approval for joint indications, which is something every patient should know before consenting to treatment.
You can review a detailed procedure overview to understand what our process looks like. For additional context on how biologic treatments compare, the PRP vs cortisone outcomes comparison is a useful read.
“Ultrasound guidance during injection is not optional, it is essential. Accuracy of placement directly affects whether the cells reach the target tissue.”
Pro Tip: Ask your provider whether ultrasound guidance is used during the injection. Blind injections, where the provider relies on landmarks rather than imaging, carry a higher risk of inaccurate placement and reduced effectiveness.
Return to activity varies. Most patients can walk the same day but should avoid high-impact activity for two to four weeks. Full return to sport typically takes six to twelve weeks, depending on the joint and the severity of the original injury.
Common pitfalls and maximizing success: Dos, don’ts, and follow-up
Even the best stem cell treatment can underperform if recovery is mismanaged. Here are the most common mistakes and how to avoid them.
What slows or sabotages recovery:
- Returning to high-impact activity too soon, before the cells have had time to integrate and reduce inflammation
- Skipping or rushing through physical therapy, which is one of the most critical factors in long-term outcomes
- Continuing anti-inflammatory medications after the procedure, which can suppress the very cellular activity you are trying to promote
- Expecting dramatic results within the first few weeks, when the biological process takes time to unfold
What supports the best outcomes:
- Following your provider’s post-injection protocol precisely, including activity restrictions and any prescribed exercises
- Attending all follow-up appointments so your provider can monitor your progress and adjust recommendations
- Staying consistent with physical therapy, even when early soreness makes it tempting to rest completely
- Maintaining open communication about any unexpected symptoms or setbacks
The evidence reinforces this point directly. Benefits for knee osteoarthritis are typically modest and short-term, making rehabilitation and post-injection care critical for maximal improvement. In other words, the injection is only one part of the equation. What you do in the weeks and months after treatment matters enormously.
“The patients who get the most out of regenerative treatment are the ones who treat recovery as seriously as training. The injection starts the process. Rehab finishes it.”
For guidance on rehab after treatment and how to compare different joint healing options, we have additional resources to help you plan your full recovery strategy.
Pro Tip: Set a 12-week check-in with your provider from the start. Mark it on your calendar before you leave the clinic. This creates accountability and gives you a structured timeline to evaluate whether the treatment is producing the expected response.
What most people get wrong about stem cell treatment for joint injuries
Here is an honest perspective that we feel compelled to share, because the marketing around regenerative medicine does not always tell the full story.
The biggest mistake active adults and athletes make is assuming that stem cell therapy is a direct replacement for surgery in every case. It is not. It is a tool, and like any tool, it works best when applied to the right problem. A focal cartilage injury in a 35-year-old runner is a very different clinical picture from bone-on-bone arthritis in a 60-year-old former football player. The same treatment applied to both patients will not produce the same result.
The truth is that marketing often outpaces the evidence. Clinics that promise dramatic, lasting cartilage regeneration in advanced arthritis cases are not being straightforward with you. The Cochrane review, one of the most rigorous forms of medical evidence synthesis, found only slight and short-lived benefits in most cases. Major specialty societies actively warn against routine use for advanced osteoarthritis.
That does not mean stem cell therapy has no value. For the right patient, at the right stage, with the right follow-through, it can meaningfully reduce pain and improve function. We have seen that firsthand in our North Texas patients. But the key phrase is “the right patient.” Honest evaluation, realistic expectations, and a commitment to rehabilitation are what separate a good outcome from a disappointing one.
We also want to address cost. Most stem cell injections are not covered by insurance. Costs can range from several hundred to several thousand dollars depending on the procedure. That financial reality makes it even more important to know upfront whether you are a strong candidate. Spending money on a treatment that is unlikely to help your specific condition is not a decision we would ever encourage.
If you are weighing your options carefully, choosing your best option starts with an honest conversation about your diagnosis, your goals, and what the evidence actually supports for your situation.
Explore your non-surgical joint recovery options with Nortex
At Nortex Tissue Regeneration, we work with active adults and athletes across North Texas who want real answers, not just hopeful promises. Our team evaluates each patient individually, using imaging, clinical history, and a thorough understanding of your activity goals to determine whether stem cell therapy, platelet-rich plasma therapy, or another biologic approach is the right fit. We believe in evidence-based care, transparent conversations about what treatment can and cannot do, and personalized protocols designed to get you back to the activities you love. If you are ready to take the next step, we invite you to learn about stem cell therapy and schedule a consultation with our team today.
Frequently asked questions
How long do stem cell injections for joints actually last?
Evidence suggests any benefit is small and most evident by six months, with unclear long-term advantages beyond that point. Managing expectations around duration is an important part of the pre-treatment conversation.
Is stem cell therapy suitable for advanced bone-on-bone arthritis?
It is generally not recommended for advanced OA per major specialty guidance, due to a lack of supporting evidence and the significant costs involved. Patients with advanced arthritis may be better served by other treatment pathways.
Are stem cell injections FDA approved for knee cartilage repair?
Only surgical cell therapy implants like MACI are FDA approved for certain knee cartilage defects. Standard office-based stem cell injections are not FDA approved for joint indications.
Can stem cells regrow cartilage in worn-out joints?
Current evidence does not support routine cartilage regrowth using stem cell injections in advanced arthritis cases. The primary benefit observed is modest pain and function improvement, not structural regeneration.